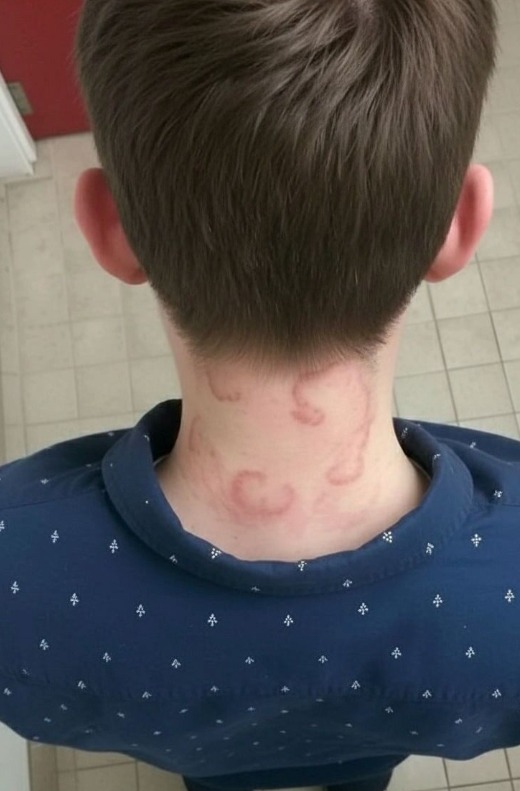
What began as a harmless itch soon revealed itself as a frightening lesson in how aggressive urticaria can be when left unchecked. At first, it was easy to dismiss—an irritating sensation on the skin, the kind most people chalk up to an allergy, a bite, or stress. But within hours, raised red weals began to appear, spreading across his body in irregular patterns. They burned and itched intensely, refusing to fade the way ordinary rashes do.
These marks were more than a surface reaction. Beneath the skin, mast cells were releasing a surge of chemicals into his bloodstream, triggering inflammation and causing tiny blood vessels to leak fluid into surrounding tissue. The result was swelling that grew rapidly worse. What looked cosmetic on the outside was actually a systemic reaction unfolding within.
As the hours passed, the condition escalated. His lips began to swell, followed by his eyelids. The mirror reflected a face he barely recognized. When swallowing became uncomfortable, fear replaced discomfort. He realized this was no longer something to “wait out.” Angio-oedema—deeper swelling beneath the skin—had set in, and the risk was no longer limited to appearance. Swelling near the mouth and throat can become dangerous quickly, interfering with breathing and signaling a medical emergency.
Doctors moved swiftly to stabilize the situation and identify possible triggers. Urticaria can be notoriously difficult to pin down. Food allergies were considered first, followed by medications, recent infections, environmental exposures, and even emotional stress. Sometimes the cause is clear; often, it isn’t. Physicians had to determine whether this was acute urticaria—typically resolving within weeks—or chronic urticaria, a condition that can persist for months or even years without a clear explanation.
Treatment focused on calming the immune response and preventing further escalation. High-dose antihistamines were introduced to block the effects of histamine, the primary chemical driving the reaction. Short courses of corticosteroids were used to reduce inflammation and control severe flare-ups. Topical treatments, including cooling menthol-based creams, provided some relief from the relentless itching, though they were only a small part of the solution.
Recovery was gradual. The swelling receded, the weals faded, and normal movement and swallowing returned. But the experience left a lasting impression. He learned to monitor his body closely, to recognize early warning signs, and to avoid known triggers once they were identified. He also learned the importance of seeking immediate medical care when swelling involves the face, lips, or throat—areas where delay can carry serious consequences.
What once seemed like “just hives” became a powerful reminder that skin reactions are not always skin-deep. Urticaria can be a visible signal of deeper immune activity, one that deserves respect and prompt treatment. With proper care, awareness, and medical support, the condition can be managed—but ignoring it can turn a minor itch into a life-threatening situation. In his case, timely intervention didn’t just ease discomfort; it quietly saved his life.